Numerous studies have found a correlation between oral health and optimal ageing and diseases, but why does this happen? And how does it work?
Normally the body’s natural defences and good oral health care, such as daily brushing and flossing, keep bacteria under control. However, without proper oral hygiene, bacteria can reach levels that might lead to oral infections, such as tooth decay and gum disease.
Gum disease is where the gums becomes red, swollen and sore, and bleed. It’s very common, but it’s important to get it checked by a dentist.
This disease is caused by a build-up of plaque on the teeth. If you don’t remove plaque from your teeth by brushing and cleaning in between them regularly, it builds up and irritates your gums.
Pete Williams, founder of Functional Medicine Associates, said: “If you look at the literature, it shows that over 50 per cent of the population over 30 in western societies have gum disease. It means that one in two patients are probably gonna have gum disease, and that’s problematic.”
Oral health is important for maintaining general health among patients and in particular the elderly.
Martijn Verhulst, Medical Liaison Manager at Sunstar, explained the relation between wellness in elderly adults and oral health: “A good example is how a gradual decline in oral function due to ageing can impact general well-being, and vice versa. Starting in Japan, the scientific community is more and more accepting that this gradual decline in oral function is part of a broader concept called physical “frailty”.”
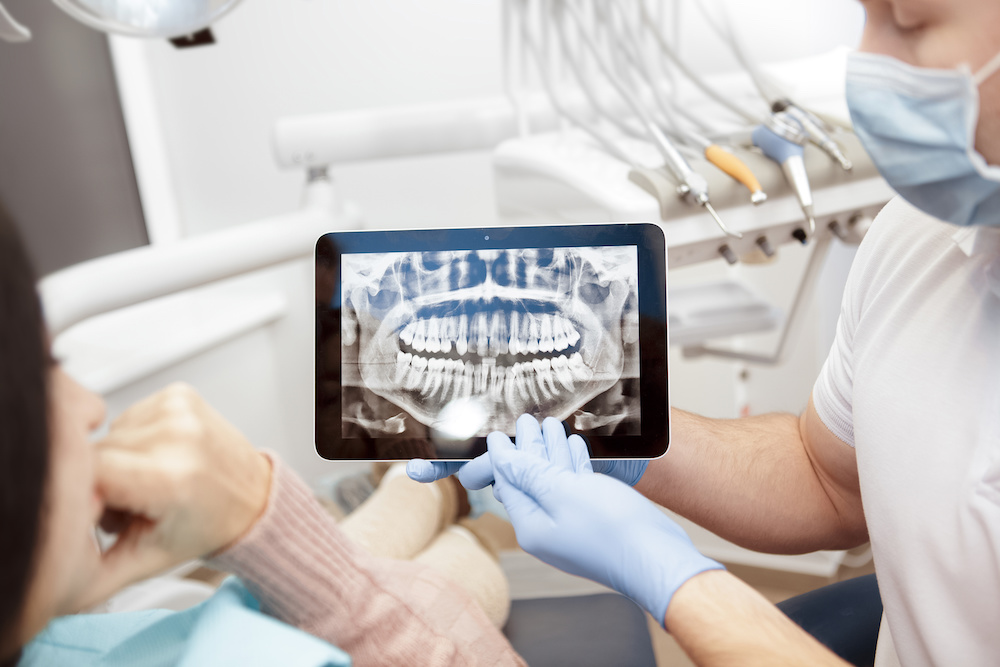
Discussing issues. Cropped shot of a professional dentist showing jaws and teeth x-rays to his patient using a digital tablet technology gadget online
As explained by Dr. Williams, having a gum disease means having a barrier that’s been broken. If a patient’s gums are bleeding or if the patient has gum recession, there is a weakness in the barriers that protect them from the outside world.
As a consequence, the bacteria can slip in the body and cause problems. With bacteria always coming through the gum, there’s a constant response from the immune system, which damages other structures at the same time.
“In addition to the effect of physical frailty on oral health, the reverse is also true,” said Verhulst. “Research has also shown a clear relationship between poor oral health and physical frailty. Problems such as losing teeth, deterioration of oral motor skills, chewing and swallowing issues, saliva disorders, and oral pain all contribute to becoming frail.
“And then finally, there’s the more patient-centred side of the relationship. Both oral and physical frailty are also associated with poor quality of life, as people start losing their independency and become less and less socially engaged due to their symptoms.”
Gum disease has also been found related to chronic diseases such as Alzheimer’s. Dr. Williams explained that what is important to understand is that a local problem becomes a systemic problem.
Therefore, an infection can travel from the mouth, possibly becoming a causative effect of what happens in the brain.
“There are some drug trials happening now, creating a drug that is an inhibitor for one of the toxic effects of the oral bacterias,” he said.
“If you control some of the pathogenic bacteria in the mouth you reduce the risk of Alzheimer’s.”
Martijn Verhulst explained that prevention is the most important thing to do. He added: “Efforts should be targeted at retaining as many teeth as possible by optimising oral hygiene and regular dentist visits.
“If a full denture is needed, it’s better to go for an implant-supported one rather than a removable one.
“When it comes to maintaining oral function, there are some studies showing that an oral and physical exercise program can improve oral hypo function. And finally, maintaining a healthy diet and an active social life are absolutely crucial for preventing oral frailty.”