Research
Alzheimer’s more common among older people who had Covid-19, study finds

A new study suggests that Covid-19 may improve the risk of Alzheimer’s in older people.
The research, published in the Journal of Alzheimer’s Disease, analysed over six million adults aged 65 or older with no prior Alzheimer’s disease diagnosis.
The study does not show that Covid-19 causes Alzheimer’s, but it adds to the growing body of research drawing links between coronavirus infection and cognitive function.
Dr. David Holtzman, a neurologist from the Washington University School of Medicine, said: “In the Alzheimer’s disease brain, the pathology starts to build up about 20 years before the symptoms begin.
“The brain has its own immune response to the pathology that’s involved in [Alzheimer’s] disease progressing.
“When there are other things that cause inflammation that are in the body that can affect the brain, likely what happens is that can even amplify the process that’s already going on.”
The study authors identified this work as a call for more research on the underlying mechanisms of Alzheimer’s disease that might explain the association.
Dr. Eliezer Masliah, director of the division of neuroscience at the National Institutes of Health’s National Institute on Aging, said: “In the next couple of years, we’re going to have a lot of very important information.
“Imagine how many millions of people over the age of 60 or 65, like myself, have had Covid. Say five per cent of them or ten per cent of them or even one per cent of them are at risk.
“We’re looking at a lot of people in the next few years that might add to the already very large epidemic of Alzheimer’s disease that we have.”
The limitations of the study include the retrospective and observational nature of the study that could introduce potential biases and Alzheimer’s disease diagnosis inaccuracy, which may not have affected the relative risk analyses considerably since both groups were formed from the same dataset.
News
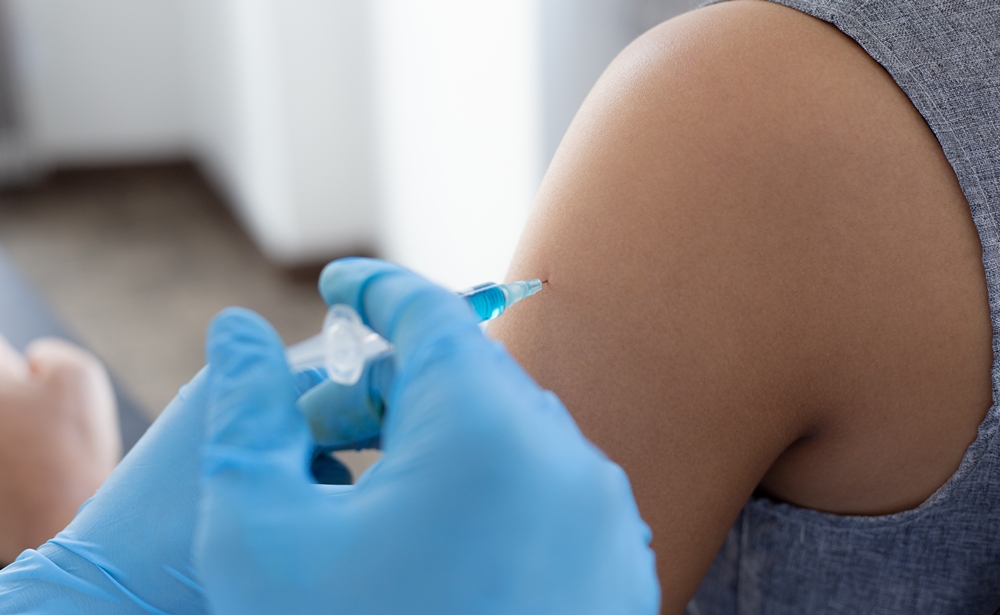
Shingles vaccine may slow biological ageing in older adults
News
Blood sugar spike after meals may increase Alzheimer’s risk

Sharp rises in blood sugar after meals may raise Alzheimer’s risk, according to genetic analysis of more than 350,000 adults.
The findings point to after-meal glucose, rather than overall blood sugar, as a possible factor in long-term brain health.
Researchers examined genetic and health data from over 350,000 UK Biobank participants aged 40 to 69, focusing on fasting glucose, insulin, and blood sugar measured two hours after eating.
The team used Mendelian randomisation, a genetic method that helps test whether biological traits may play a direct role in disease risk.
People with higher after-meal glucose had a 69 per cent higher risk of Alzheimer’s disease.
This pattern, known as postprandial hyperglycaemia (elevated blood sugar after eating), stood out as a key factor.
The increased risk was not explained by overall brain shrinkage (atrophy) or white matter damage, suggesting after-meal glucose may affect the brain through other pathways not yet fully understood.
Dr Andrew Mason, lead author, said: “This finding could help shape future prevention strategies, highlighting the importance of managing blood sugar not just overall, but specifically after meals.”
Dr Vicky Garfield, senior author, added: “We first need to replicate these results in other populations and ancestries to confirm the link and better understand the underlying biology.
“If validated, the study could pave the way for new approaches to reduce dementia risk in people with diabetes.”
Insights
Study reveals why memory declines with age

A recent international study that pooled brain scans and memory tests from thousands of adults has shed new light on how structural brain changes are tied to memory decline as people age.
The findings show that the connection between shrinking brain tissue and declining memory is nonlinear, stronger in older adults, and not solely driven by known Alzheimer’s-associated genes like APOE ε4.
This suggests that brain ageing is more complex than previously thought, and that memory vulnerability reflects broad structural changes across multiple regions, not just isolated pathology.
Alvaro Pascual-Leone, MD, PhD is senior scientist at the Hinda and Arthur Marcus Institute for Aging Research and medical director at the Deanna and Sidney Wolk Center for Memory Health.
The researcher said: “By integrating data across dozens of research cohorts, we now have the most detailed picture yet of how structural changes in the brain unfold with age and how they relate to memory.”
The study found that structural brain change associated with memory decline is widespread, rather than confined to a single region.
While the hippocampus showed the strongest association between volume loss and declining memory performance, many other cortical and subcortical regions also demonstrated significant relationships.
This suggests that cognitive decline in ageing reflects a distributed macrostructural brain vulnerability, rather than deterioration in a few specific brain regions.
The pattern across regions formed a gradient, with the hippocampus at the high end and progressively smaller but still meaningful effects across large portions of the brain.
Importantly, the relationship between regional brain atrophy and memory decline was not only variable across individuals but also highly nonlinear.
Individuals with above-average rates of structural loss experienced disproportionately greater declines in memory, suggesting that once brain shrinkage reaches higher levels, cognitive consequences accelerate rather than progress evenly.
This nonlinear pattern was consistent across multiple brain regions, reinforcing the conclusion that memory decline in cognitively healthy ageing is linked to global and network-level structural changes, with the hippocampus playing a particularly sensitive role but not acting alone.
Pascual-Leone said: “Cognitive decline and memory loss are not simply the consequence of ageing, but manifestations of individual predispositions and age-related processes enabling neurodegenerative processes and diseases.
“These results suggest that memory decline in ageing is not just about one region or one gene — it reflects a broad biological vulnerability in brain structure that accumulates over decades.
“Understanding this can help researchers identify individuals at risk early, and develop more precise and personalized interventions that support cognitive health across the lifespan and prevent cognitive disability.”

 News2 weeks ago
News2 weeks agoFDA clears automated brain fluid device

 Technology2 weeks ago
Technology2 weeks agoAgetech World’s latest innovation & investment round-up

 News2 weeks ago
News2 weeks agoInsilico signs US$888m oncology deal with Servier

 News2 weeks ago
News2 weeks agoFood preservatives linked to increased diabetes and cancer risk, study finds

 News2 weeks ago
News2 weeks agoUK bans junk food ads before 9pm to protect child health

 News1 week ago
News1 week agoCaptioning glasses win AARP pitch at CES

 Insights2 weeks ago
Insights2 weeks agoGlobal longevity initiative launches North American chapter

 News6 days ago
News6 days agoInterview: GlycanAge launch first hospital-based tests